Information about COVID-19 (Coronavirus)
On 11 March 2020 the World Health Organization confirmed COVID-19 (coronavirus) has now spread all over the world (this means it is a ‘pandemic’). Hospitals have very robust infection control procedures, however, it is impossible to make sure you don’t catch coronavirus either before you come into the hospital or once you are there. You will need to think carefully about the risks associated with the procedure, the risk of catching coronavirus while you are in hospital, and of not going ahead with the procedure at all. Your healthcare team can help you understand the balance of these risks. If you catch the coronavirus, this could affect your recovery and might increase your risk of pneumonia and even death. Talk to your healthcare team about the balance of risk between waiting until the pandemic is over (this could be many months) and going ahead with your procedure.
Please visit the World Health Organization website: www.who.int for up-to-date information.
Information about your procedure
Following the Covid-19 (coronavirus) pandemic, some operations have been delayed. As soon as the hospital confirms that it is safe, you will be offered a date. Your healthcare team can talk to you about the risks of having your procedure if you have coronavirus. It is then up to you to decide whether to go ahead or not. The benefits of the procedure, the alternatives and any complications that may happen are explained in this document. If you would rather delay or not have the procedure until you feel happy to go ahead, or if you want to cancel, tell your healthcare team.
If you decide to go ahead, you may need to self-isolate for a period of time beforehand (your healthcare team will confirm how long this will be). If you are not able to self-isolate, tell your healthcare team as soon as possible. You may need a coronavirus test a few days before the procedure. If your test is positive (meaning you have coronavirus), the procedure will be postponed until you have recovered.
Coronavirus spreads easily from person to person. The most common way that people catch it is by touching their face after they have touched anyone or anything that has the virus on it. Wash your hands with alcoholic gel or soap and water when you enter the hospital, at regular intervals after that, and when you move from one part of the hospital to another.
Even if you have had the first or both doses of a Covid vaccine, you will still need to practise social distancing, hand washing and wear a face covering when required.
If your healthcare team need to be close to you, they will wear personal protective equipment (PPE). If you can’t hear what they are saying because of their PPE, ask them to repeat it until you can. Chairs and beds will be spaced apart. You may not be allowed visitors, or your visiting may be restricted.
Your surgery is important and the hospital and health professionals looking after you are well equipped to perform it in a safe and clean environment. Guidance about coronavirus may change quickly ─ your healthcare team will have the most up-to-date information.
What is a revision total hip replacement?
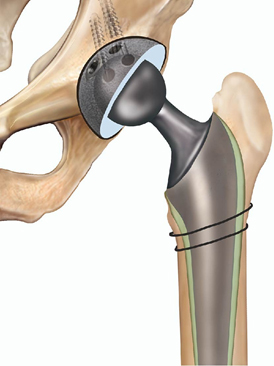
A revision total hip replacement is an operation to take out parts of your old hip replacement and put in new ones.
Your surgeon has recommended a revision total hip replacement operation. However, it is your decision to go ahead with the operation or not. This document will give you information about the benefits and risks to help you to make an informed decision.
If you have any questions that this document does not answer, it is important that you ask your surgeon or the healthcare team. Once all your questions have been answered and you feel ready to go ahead with the procedure, you will be asked to sign the informed consent form. This is the final step in the decision-making process. However, you can still change your mind at any point before the procedure.
What causes a hip replacement to fail?
A hip replacement can fail for the following reasons.
- Wearing out of the artificial ball-and-socket joint – This releases tiny bits of material that can cause damage to the bone and soft tissues around the joint or can cause the joint to come loose from the
- Infection in your hip replacement – Infection can make your hip replacement come loose from the
- Dislocation (coming out of joint) – You may decide to have an operation to try to prevent this from happening
- Fracture (break) of the femur around your hip replacement – This can happen if you fall heavily on your
These problems can make it difficult for you to walk, and sometimes cause pain. Your surgeon will discuss with you why they have recommended a revision total hip replacement.
What are the benefits of surgery?
You should be able to walk better and do more of your normal activities.
Are there any alternatives to surgery?
If your hip replacement is wearing out, it may only be happening slowly. If your symptoms are mild, you and your surgeon may decide to watch and wait for a while. You will need to have regular
x-rays.
If you have an infection in your hip replacement, using antibiotics over the long term can sometimes prevent your hip replacement from failing.
However, the infection will not usually go away completely unless your hip replacement is removed.
If your hip replacement keeps coming out of joint, you can wear a brace to try to keep your hip in place. A brace is large and may be uncomfortable.
If you have a fracture near your hip replacement but the replacement is still well fixed to the bone, you maybe able to be treated with painkillers and using walking aids until the fracture heals. This can take a long time. Sometimes you may be able to have an operation to fix the fracture without changing your hip replacement.
What will happen if I decide not to have the operation?
If your hip replacement is coming loose because of wear or infection, it will probably get more painful over time. The bone around a loose hip replacement can get thin and it may break (fracture). You will need to have a major operation to fix the fracture and do your hip replacement again.
If you have an infection in your hip replacement, it can spread to other places around your body, including other artificial joints and vital organs.
Your surgeon will discuss with you what is likely to happen.
What does the operation involve?
The healthcare team will carry out a number of checks to make sure you have the operation you came in for and on the correct side. You can help by confirming to your surgeon and the healthcare team your name and the operation you are having.
Various anaesthetic techniques are possible. Your anaesthetist will discuss the options with you. You may be given antibiotics during the operation to reduce the risk of infection.
Your surgeon will make a cut on the side of your hip. They will remove your hip replacement and any cement. This often takes a long time and can be difficult.
Your surgeon will put in a new hip replacement, which is often larger than your old one. Your hip replacement is fixed into the bone using acrylic cement or special coatings on your hip replacement that bond directly to the bone.
Your surgeon will close your skin with stitches or clips.
The type of surgery you need can be more complicated if the bone is thin or broken, or if you have an infection. Your surgeon will discuss with you what the operation is likely to involve.
- If your bone is thin or has broken, they may need to build it up with a bone graft, special wire mesh and cables, or a metal
- If you have an infected hip replacement, you may need to have two separate In the first, your surgeon will remove your old hip replacement, any cement and all infected material. They will put antibiotics in your hip and you will also need antibiotic injections for several weeks. An infection may take 2 to 3 months to go completely. You will need a second operation to put in the new hip replacement.
What should I do about my medication?
Make sure your healthcare team knows about all the medication you take and follow their advice. This includes all blood-thinning medication as well as herbal and complementary remedies, dietary supplements, and medication you can buy over the counter.
What can I do to help make the operation a success?
If you smoke, stopping smoking now may reduce your risk of developing complications and will improve your long-term health.
Try to maintain a healthy weight. You have a higher risk of developing complications if you are overweight.
Regular exercise should help to prepare you for the operation, help you to recover and improve your long-term health. Before you start exercising, ask the healthcare team or your GP for advice.
You can reduce your risk of infection in a surgical wound.
- In the week before the operation, do not shave or wax the area where a cut is likely to be
- Try to have a bath or shower either the day before or on the day of the
- Keep warm around the time of the Let the healthcare team know if you feel cold.
- If you are diabetic, keep your blood sugar levels under control around the time of your
If you have not had the coronavirus (Covid-19) vaccine yet, ask your healthcare team if this can be done before your operation. This will reduce your risk of serious illness related to Covid-19 while you recover.
What complications can happen?
The healthcare team will try to reduce the risk of complications.
Any numbers which relate to risk are from studies of people who have had this operation. Your doctor may be able to tell you if the risk of a complication is higher or lower for you.
Some complications can be serious.
You should ask your doctor if there is anything you do not understand.
Your anaesthetist will be able to discuss with you the possible complications of having an anaesthetic.
General complications of any operation
- Bleeding during or after the You may need a blood transfusion.
- Infection of the surgical site (wound). It is usually safe to shower after 2 days but you should check with the healthcare team. Keep your wound dry and Let the healthcare team know if you get a high temperature, notice pus in your wound, or if your wound becomes red, sore or painful. An infection usually settles with antibiotics but you may need special dressings and your wound may take some time to heal. In some cases another operation might be needed. Do not take antibiotics unless you are told you need them.
- Allergic reaction to the equipment, materials or The healthcare team is trained to detect and treat any reactions that might happen. Let your doctor know if you have any allergies or if you have reacted to any medication or tests in the past.
- Acute kidney injury. A significant drop in your blood pressure during the operation can damage your kidneys. The healthcare team will monitor your condition closely to reduce the chance of this Any kidney damage is usually short lived although some people may need to spend longer in hospital and a small number can go on to develop chronic kidney disease that may require dialysis.
- Blood clot in your leg (deep-vein thrombosis – DVT) (risk: 1 in 25). This can cause pain, swelling or redness in your leg, or the veins near the surface of your leg to appear larger than normal. The healthcare team will assess your risk. They will encourage you to get out of bed soon after the operation and may give you injections, medication, or inflatable boots or special stockings to Let the healthcare team know straight away if you think you might have a DVT.
- Blood clot in your lung (pulmonary embolus), if a blood clot moves through your bloodstream to your lungs (risk: 1 in 100). Let the healthcare team know straight away if you become short of breath, feel pain in your chest or upper back, or if you cough up blood. If you are at home, call an ambulance or go immediately to your nearest Emergency
- Difficulty passing urine. You may need a catheter (tube) in your bladder for 1 to 2
- Chest infection. You may need antibiotics and If you have the operation within 6 weeks of catching Covid-19, your risk of a chest infection is increased (see the ‘Covid-19’ section for more information).
- Heart attack (where part of the heart muscle dies) (risk: 1 in 200). A heart attack can sometimes cause
- Stroke (loss of brain function resulting from an interruption of the blood supply to your brain). A stroke can sometimes cause
Specific complications of this operation
- Split in the femur, if the bone is weak. Your surgeon may need to insert some wires around the femur, or use a different type of hip
- Damage to nerves around your hip, leading to weakness, numbness or pain in your leg or foot (risk: 1 in 75). This usually gets better but may be
- Damage to blood vessels around your hip, leading to loss of circulation to your leg and foot (risk: 1 in 1,000). You will need surgery straight away to restore the blood
- Infection in your hip, which can result in loosening and failure of your hip You will usually need one or more further operations to control the infection. If you get any kind of infection, including a dental infection, get it treated straight away as the infection could spread to your hip.
- Loosening without You may need another operation to do your hip replacement again.
- Bone forming in muscles around your hip replacement (heterotopic ossification) (risk: 1 in 2). This can cause loss of movement in your You may need another operation to remove the extra bone.
- Dislocation of your hip replacement (risk: 1 in 10). You may need another operation if it keeps on
- Leg length Your surgeon will try to make your legs the same length again but this is not always possible. You may need a shoe-raise.
- Death sometimes happens after a revision total hip replacement (risk: 1 in 70). The risk is less the fitter you
Covid-19
A recent Covid-19 infection increases your risk of lung complications or death if you have an operation under general anaesthetic. This risk reduces the longer it is since the infection. After 7 weeks the risk is no higher than someone who has not had Covid-19. However, if you still have symptoms the risk remains high. The risk also depends on your age, overall health and the type of surgery you are having.
You must follow instructions to self-isolate and take a Covid-19 test before your operation. If you have had Covid-19 up to 7 weeks before the operation you should discuss the risks and benefits of delaying it with your surgeon.
Consequences of this procedure
- The healthcare team will give you medication to control the pain and it is important that you take it as you are told so you can move about as advised.
- Unsightly scarring of your skin, although revision hip-replacement wounds usually heal to a neat
How soon will I recover?
In hospital
After the operation you will be transferred to the recovery area and then to the ward. You will usually have an x-ray to check the position of your hip replacement.
The physiotherapist will help you to start walking using crutches or a walking frame, usually the next day.
You may need to wear a brace to protect your hip. Follow the advice of the physiotherapist on how to use it. Your surgeon or the physiotherapist will tell you how much weight you can put on your leg.
Keep your wound dry for 4 to 5 days, and use a waterproof dressing when you have a bath or shower.
The healthcare team will tell you if you need to have any stitches or clips removed, or dressings changed.
You should be able to go home after 3 to 10 days. However, your doctor may recommend that you stay a little longer.
If you are worried about anything, in hospital or at home, contact the healthcare team. They should be able to reassure you or identify and treat any complications.
Returning to normal activities
To reduce the risk of a blood clot, make sure you carefully follow the instructions of the healthcare team if you have been given medication or need to wear special stockings.
The healthcare team will tell you when you can return to normal activities. To reduce the risk of problems, it is important to look after your new hip as you are told.
You may need to use a walking aid for a few weeks. It often takes longer to recover from a revision hip replacement than your first hip replacement.
Regular exercise should help you to return to normal activities as soon as possible. Before you start exercising, ask the healthcare team or your GP for advice.
Do not drive until you can control your vehicle, including in an emergency, and always check your insurance policy and with the healthcare team.
Ask your healthcare team if you need to do a Covid-19 test when you get home.
The future
Most people make a good recovery and most revision total hip replacements work well. It is important to follow the advice the physiotherapist gives you about exercises to strengthen your hip muscles. It is common for your leg to be swollen after a hip replacement. It can take up to a year for the swelling to go down.
A revision total hip replacement can fail with time, if it wears out, or the original problem comes back. You may need another operation (risk: 1 in 7 by 10 years after the operation).
You should have an x-ray of your hip replacement at least every 5 years to check for any problems.
Summary
If your original hip replacement fails, you can usually have another operation to do your hip replacement again. If this revision operation is successful, you should be able to continue many of your normal activities.
Surgery is usually safe and effective but complications can happen. You need to know about them to help you to make an informed decision about surgery. Knowing about them will also help to detect and treat any problems early.
Revision Total Hip Replacement
If you would like to have additional information on the treatment of hip arthritis or would like to learn more about total hip replacement, please contact Mr Tarique Parwez, serving the communities of Hertfordshire, Luton, Hatfield.
